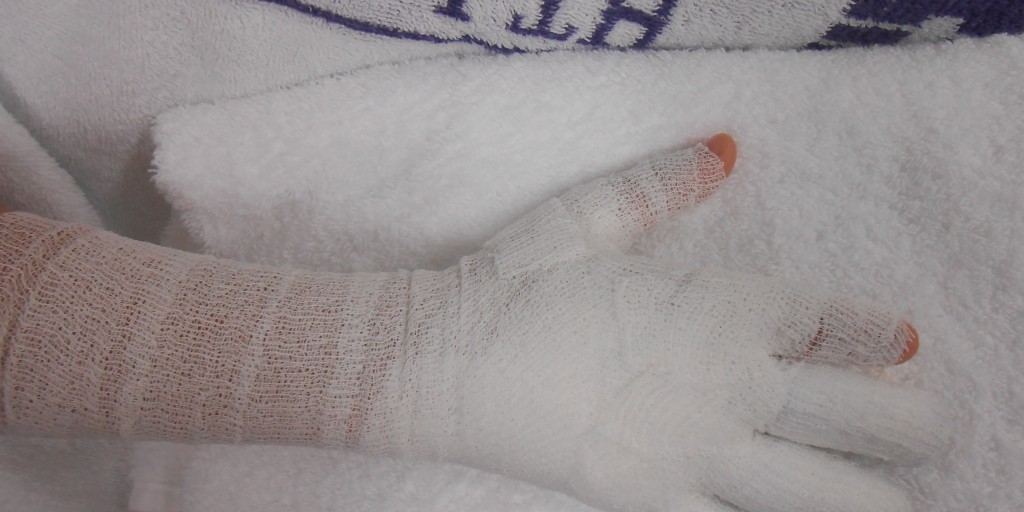
Oedema management: compression bandaging
How:
- Compression bandaging is used to shift accumulated fluid within the extracellular space, back within blood capillaries and into peripheral circulation.
- Lower limb compression bandaging used after skin grafting when clearance has been given to have legs in a dependent position is used to avoid venous pooling which can contribute to graft sloughing [4]
- Take measurements prior to bandaging of both the affected and unaffected limb (where possible). This will allow monitoring of the effectiveness of the bandaging
- Select appropriate bandaging materials (High Stretch vs. Low Stretch) based on your knowledge of child’s oedema, child’s age, functional activity, level arousal and burn history.
- Apply compression over dressings in graduated manner to ensure fluid moving distally to proximally.
- Bandaging overlap will depend on the child’s tolerance of compression bandaging and amount of oedema present. Read product recommendations prior to applying.
- Apply padding to exposed bony prominences to protect underlying skin integrity and to remainder of limb prior to compression bandage to ensure even, graduated compression.
- End the compression bandage at the joint beyond the area of oedema.
Regime:
- Will depend on oedema present and child’s tolerance of bandaging.
- Compression bandaging is typically applied 24/24 in healing burns and replaced at time of next dressing change or earlier (i.e. too loose).
Bandaging tips and tricks:
- Some bandages will impact fluid transfer of the dressing so consult with nursing staff before commencing.
- Highlight the end of cohesive bandages to make it easier to see your figure 8/spiral formation when applying.
- Consider the impact of bandaging on the child’s occupations and ways to protect during self-care tasks/feeding (i.e. wrap with gladwrap when feeding, winter glove over top).

- Seek clearance from medical team prior to commencing compression bandaging
- Ensure the child has no contraindications for compression.

- Close monitoring is required after application compression to ensure nil compromise to circulation.
- Use of webspacers (e.g. strips of foam/dressing) can be placed between digits to prevent distal fluid collection.
- Consider the child’s developmental stage and ability to report pain or altered sensations.
- Provide written and verbal education to parents about precautions of use, how to monitor circulation, correct application at home and what to do if any signs of circulation compromise. Parents MUST continue to do this at home whilst the child is awake and asleep.

